Roy A. Rothman, DPM, PA
Podiatric Medicine and SurgeonFoot & Ankle Specialist


High ankle pain, which is often referred to as a syndesmotic ankle sprain, occurs when the ligaments connecting the tibia and fibula are injured. This type of lower leg bone injury typically happens when the ankle is twisted forcefully, which causes the ligaments to stretch or tear. Athletes, especially those involved in sports like football and skiing, are more prone to incurring high ankle sprains. Symptoms can include less swelling than typical ankle sprains, difficulty moving the ankle up and down, and trouble bearing weight on the affected leg. Sometimes bruising appears a few days after the injury. It is important to differentiate high ankle sprains from other conditions like fractures or regular ankle sprains to ensure proper treatment. If you experience persistent ankle pain, difficulty walking, or notice swelling and bruising after an injury, it is suggested that you schedule an immediate appointment with a podiatrist for a diagnosis and treatment plan.
Although ankle sprains are common, they aren’t always minor injuries. If you need your ankle injury looked at, contact Roy Rothman, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains are the result of a tear in the ligaments within the ankle. These injuries may happen when you make a rapid shifting movement while your foot is planted. A less common way to sprain your ankle is when your ankle rolls inward while your foot turns outward.
What Are the Symptoms?
Preventing a Sprain
Treatment of a Sprain
In many cases, the RICE method (Rest, Ice, Compression, and Elevate) is used to treat ankle sprains. However, you should see a podiatrist to see which treatment option would work best with your injury. In severe cases, surgery may be required.
It is important to ask your doctor about rehab options after you receive treatment for your injury. Stretching, strength training, and balance exercises may help the ankle heal while also preventing further injury.
If you have any questions, please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
An ankle sprain occurs when one or more ankle ligament gets overly stretched. Ligaments are strong bands of tissue that bind and support the bones and other structures that make up the ankle. In more severe ankle sprains, the ligament(s) tear—either partially or completely—and there may be an audible popping noise at the moment of injury.
Ankle sprains are quite common and can occur when the ankle rolls outwardly (eversion) or inwardly (inversion), causing the ligament(s) to stretch beyond normal limits, or even tear. Falls, twists, or blows to the ankle during sports or other activities can cause this injury, as well as wearing improper footwear, running on uneven surfaces, or having weak ankles.
Depending on the injury’s severity, an ankle sprain will be classified as Grade I, Grade II, or Grade III. Grade I sprains involve ligament(s) being overly stretched but not torn, with symptoms of mild pain, swelling, and ankle instability. There may also be some difficulty bearing weight. A Grade II sprain usually involves a partial tear of the ligament which brings more intensity in these symptoms, along with possible bruising. With a Grade III sprain, the ligament is completely torn, the symptoms are severe, and it may not be possible to put weight on the affected foot at all.
To diagnose and grade an ankle sprain, a podiatrist will perform a physical examination, checking for tenderness and range of motion in the ankle. For more severe sprains, X-rays or other imaging studies may be necessary.
It is vitally important to have an ankle sprain treated properly as improper healing often leads to future ankle sprains and possibly even chronic ankle stability. Treatment for an ankle sprain will vary, depending on its severity, and may include the RICE method (Rest/Ice/Compression/Elevation), physical therapy, bracing, medications, and possibly even surgery to repair a torn ligament. Rehabilitation is very important for the sprain to heal properly and to restore functionality.
 Plantar fasciitis is a condition that results in heel pain. It happens when the plantar fascia, a thick band of tissue running across the bottom of your foot and connecting your heel bone to your toes, becomes inflamed. This inflammation can cause sharp, stabbing pain, particularly noticeable with your first steps in the morning or after long periods of rest. Customized foot orthotics can reduce the heel pain associated with plantar fasciitis by providing targeted support and cushioning to the foot. These tailored inserts fit into your shoes to distribute pressure more evenly across the foot, reduce strain on the plantar fascia, and correct any abnormal walking patterns that could be contributing to the pain. Customized orthotics can significantly alleviate uncomfortable heel pain from plantar fasciitis and help prevent its recurrence, especially because it is a solution tailored to your specific foot problems. If you are experiencing heel pain from plantar fasciitis, it is suggested that you visit a podiatrist, who can determine if customized orthotics are the right course of treatment for you.
Plantar fasciitis is a condition that results in heel pain. It happens when the plantar fascia, a thick band of tissue running across the bottom of your foot and connecting your heel bone to your toes, becomes inflamed. This inflammation can cause sharp, stabbing pain, particularly noticeable with your first steps in the morning or after long periods of rest. Customized foot orthotics can reduce the heel pain associated with plantar fasciitis by providing targeted support and cushioning to the foot. These tailored inserts fit into your shoes to distribute pressure more evenly across the foot, reduce strain on the plantar fascia, and correct any abnormal walking patterns that could be contributing to the pain. Customized orthotics can significantly alleviate uncomfortable heel pain from plantar fasciitis and help prevent its recurrence, especially because it is a solution tailored to your specific foot problems. If you are experiencing heel pain from plantar fasciitis, it is suggested that you visit a podiatrist, who can determine if customized orthotics are the right course of treatment for you.
Many people suffer from bouts of heel pain. For more information, contact Roy Rothman, DPM of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in DeBary, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Have you ever gotten up from a chair or out of bed in the morning, and upon taking that first step, feel like your heel has stepped on a tack? Many people experience a feeling of sharp pain which radiates into their arch from their heel and which does not allow them to put their heel on the floor. Sometimes they need to sit back down, stand only on their toes and use the wall for balance. If you can take a few steps, it seems to go away and lessen, allowing you to then resume your activity. Later, throughout your day and after a period of rest, it can happen again. If this sounds familiar you may be suffering from your first attack of heel pain.
Heel pain is a debilitating condition that affects day to day activities. Running and walking both causes stress on the heel because the heel is the part of the foot that hits the ground first. This means that the heel is taking on your entire weight. Diagnosis and treatments for heel pain can be easily found through your podiatrist.
Plantar Fasciitis
One of the main causes of heel pain is a condition known as plantar fasciitis. The plantar fascia is a band of tissue that extends along the bottom of the foot, from the toe to the bottom of the heel. A rip or tear in this ligament can cause inflammation of these tissues, resulting in heel pain. People who do not wear proper fitting shoes are often at risk of developing problems such as plantar fasciitis. Unnecessary stress from ill-fitting shoes, weight change, excessive running, and wearing non-supportive shoes on hard surfaces are all causes of plantar fasciitis.
Achilles Tendonitis
Achilles tendonitis is another cause of heel pain. Similar to plantar fasciitis, inflammation of the Achilles tendon will cause heel pain due to stress fractures and muscle tearing. A lack of flexibility of the ankle and heel is an indicator of Achilles tendonitis. If left untreated, this condition can lead to plantar fasciitis and cause even more pain on your heel.
Heel Spur
A third cause of heel pain is a heel spur. A heel spur occurs when the tissues of the plantar fascia undergo a great deal of stress, leading to a separation of the ligament from the heel bone entirely. This results in a pointed fragment of bone on the ball of the foot, known as a heel spur.

Your feet work hard each day to support your body and facilitate movement, and for that reason, it makes sense to keep them in shape through regular exercise. Engaging in simple foot exercises is one way to do just that. Regularly performing toe raises, curls, splay movements and stretches can improve flexibility and range of motion. These exercises also help to reduce foot and ankle pain as well as muscle soreness, while enhancing your overall foot health. By incorporating foot exercises into your routine daily, or even three days a week, you can strengthen the muscles, tendons, and ligaments in your feet. This in turn promotes better balance, stability, and posture. Activities like marble pickups and tennis ball rolls not only strengthen muscles but also enhance coordination and may reduce the risk of falls, particularly in older adults. However, it is essential to listen to your body and avoid overexertion, ensuring a gentle and consistent approach to foot exercises. It is suggested that you schedule an appointment with a podiatrist who can provide guidance on suitable exercises tailored to your specific needs and foot conditions.
Exercising your feet regularly with the proper foot wear is a great way to prevent injuries and build strength. If you have any concerns about your feet, contact Roy Rothman, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Exercise for Your Feet
Exercise for your feet can help you gain strength, mobility and flexibility in your feet. They say that strengthening your feet can be just as rewarding as strengthening another part of the body. Your feet are very important, and we often forget about them in our daily tasks. But it is because of our feet that are we able to get going and do what we need to. For those of us fortunate enough to not have any foot problems, it is an important gesture to take care of them to ensure good health in the long run.
Some foot health exercises can include ankle pumps, tip-toeing, toe rises, lifting off the floor doing reps and sets, and flexing the toes. It is best to speak with Our doctor to determine an appropriate regimen for your needs. Everyone’s needs and bodies are different, and the activities required to maintain strength in the feet vary from individual to individual.
Once you get into a routine of doing regular exercise, you may notice a difference in your feet and how strong they may become.
If you have any questions please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Foot and ankle pain can be a nuisance in a person’s life, especially if it happens frequently. The best way to prevent this type of pain, is to exercise often. Regular exercise of the foot includes stretching and strength exercises. Stretching exercises can help prevent injuries such as a sprained ankle, while strength exercises can prevent ailments such as plantar fasciitis.
Stretching exercises can help improve flexibility and the foot and ankle’s range of motion. These exercises can certainly help with those who participate in high-energy activities such as sports. Many athletes routinely perform foot and ankle exercises to prevent injuries like sprained ankles, which are common injuries where the tendons in the ankle are over stretched. Strength exercises help develop foot muscles for better support and protection.
Most exercises are simple and can be done at home, either standing or sitting. One chair exercise is called “limber up”. In this exercise, a person would start by sitting down with their feet flat on the floor. Then lift one leg up so the feet are not touching the floor, then rotate your foot clockwise 15-20 times, and 15-20 times counterclockwise. Repeat the same process with the opposite leg. Another sitting exercise helps stretch the back of your heel and requires an exercise band. It begins by looping the band around a heavy piece of furniture, or something stable that will not be moved when the band is tugged or pulled. Then sit directly in front of it, and slide one foot into the loop, so that the band curves around the forefoot. Start by pulling the forefoot back and holding it for 5-10 seconds. Doing this 10-15 times on each foot, will stretch the back of your heel, increasing your flexibility.
Foot exercises that require standing are also just as easy and simple. Referred as the “Achilles Stretch”, this exercise stretches the Achilles tendon, making it more flexible, helping prevent foot, ankle, and leg pain. It begins by first standing and facing the wall, with the arms outstretched and the palms on the wall. Then place one foot behind another keeping the back leg straight, and the forward leg bending at the knee. Make sure both heels are flat on the floor and adjust your stance accordingly. With your hips, lean forward to feel the stretch, you can also adjust the distance from your feet to feel the stretch in various parts of the calf. Make sure to hold the stretch for about 30 seconds and repeat the same process 3 times with each leg. An even easier foot exercise is simply walking on sand. Walking barefoot on sand both strengthens and stretches your feet.
Doing these exercises regularly can help prevent many foot and ankle problems. Other foot exercises can even relieve pain. For example, those affected with plantar fasciitis can simply sit down on a chair, and then place a tennis ball below their affected foot. By rolling the ball under the foot, and increasing or decreasing pressure, pain will be relieved. With any exercise, it is always important to do a small warmup such as walking a few laps around the house to get the blood flowing. If after doing an exercise to relieve pain such as the tennis ball exercise, or are unsure that your execution is correct, be sure to contact a podiatrist for further instruction.
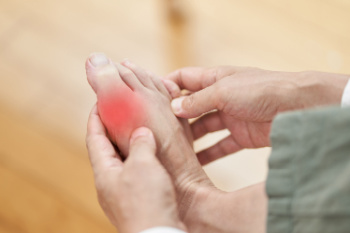
Experiencing sudden joint pain, swelling, and redness in your big toe? It could be gout, a condition where urate crystals accumulate in the joints. To determine whether you have gout, a podiatrist may recommend various tests. Blood tests are essential to check uric acid levels, although elevated levels don't always signify gout. Joint fluid testing, or arthrocentesis, involves extracting fluid from the affected joint to identify uric acid crystals, confirming a gout diagnosis. Ultrasound imaging can reveal inflammation and the presence of crystals, or tophi, around the joint. Additionally, dual-energy computerized tomography, or DECT, scans provide detailed images to show uric acid crystals within the joints, aiding in diagnosis. If you're experiencing severe and persistent discomfort in the big toe joint, it is suggested that you make an appointment with a podiatrist. This foot doctor is medically trained to diagnose symptoms of gout and offer the appropriate options to manage this condition.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Roy Rothman, DPM from Florida. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
Risk Factors
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Gout is a form of arthritis that is caused by a buildup of uric acid crystals in the joints. This considered to be one of the most frequently recorded medical illnesses throughout history. Gout occurrences in the US have risen within the past twenty years and the condition now affects 8.3 million people which is 4% of all Americans. Researchers have found that gout affects men more than women and African-American men more than white men.
Symptoms of gout are warmth, swelling, discoloration, and tenderness in the affected joint area. The small joint on the big toe is the most common place for a gout attack to occur.
People who are obese, gain weight excessively, drink alcohol heavily, have high blood pressure, or have abnormal kidney function are more likely to develop gout. Furthermore, certain drugs and diseases are likely to increase levels of uric acid in the joints which eventually leads to gout. You are also more likely to develop gout if you eat a lot of meat and fish.
Many who experience gout attacks will experience repeated attacks over the years. Some people who have gout symptoms, may never have them again, but others may experience them several times a year. If you have gout symptoms throughout the year, you may have recurrent gout. Those who have gout should also be careful about their urate crystals collecting in their urinary tract, because this may lead to kidney stones.
Diagnosis for gout is done by checking the level of uric acid in the joints and blood. Your podiatrist may also prescribe medicine to reduce uric acid buildup in the blood, which will help prevent any gout attacks.
To treat gout, your podiatrist may also prescribe you Anti-inflammatory medication (NSAIDs) which will relieve the pain and swelling of a gout episode and it can also shorten a gout attack. Maintaining a healthy diet is also a proven method to prevent gout attacks.

In-toeing in your child is a foot deformity where the front half of the foot bends or turns inward toward the side of the big toe. This condition, known as metatarsus adductus, can be attributed to the baby's positioning in the womb. Family history can also play a role. Symptoms of metatarsus adductus typically include inward angulation of the front part of the foot, with ankles and heel in a normal position. In-toeing, or walking with the forefoot turned in, can result from this deformity. Diagnosis is typically made after a physical exam, with an additional assessment of the hips to rule out other issues. Although metatarsus adductus may correct itself with time, performing certain stretching exercises, wearing splints, special shoes, or a cast may be treatments prescribed by a podiatrist. The type of intervention is generally based on the flexibility of the foot. Surgery is rarely needed for in-toeing, and is usually postponed until the child is older. Despite their in-toeing, most children can still engage in athletic activities later in life without interference. To find out more about managing your child's in-toeing, it is suggested that you schedule an appointment with a podiatrist.
Congenital foot problems require immediate attention to avoid future complications. If you have any concerns, contact Roy Rothman, DPM of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Congenital foot problems are deformities affecting the feet, toes, and/or ankles that children are born with. Some of these conditions have a genetic cause while others just happen. Some specific foot ailments that children may be born with include clubfeet, polydactyly/macrodactyly, and cleft foot. There are several other foot anomalies that can occur congenitally. What all of these conditions have in common is that a child may experience difficulty walking or performing everyday activities, as well as trouble finding footwear that fits their foot deformity. Some of these conditions are more serious than others. Consulting with a podiatrist as early as possible will help in properly diagnosing a child’s foot condition while getting the necessary treatment underway.
What are Causes of Congenital Foot Problem?
A congenital foot problem is one that happens to a child at birth. These conditions can be caused by a genetic predisposition, developmental or positional abnormalities during gestation, or with no known cause.
What are Symptoms of Congenital Foot Problems?
Symptoms vary by the congenital condition. Symptoms may consist of the following:
Treatment and Prevention
While there is nothing one can do to prevent congenital foot problems, raising awareness and receiving neonatal screenings are important. Early detection by taking your child to a podiatrist leads to the best outcome possible.
If you have any questions please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.