
Roy A. Rothman, DPM, PA
Podiatric Medicine and SurgeonFoot & Ankle Specialist



Plantar warts, though often considered minor nuisances, hold interesting facts worth exploring. These warts, caused by the human papillomavirus, or HPV, commonly appear on the soles of the feet, particularly in areas subjected to pressure or friction. Unlike other warts, plantar warts grow inward due to the pressure exerted by walking, leading to a flattened appearance. They may present as small, grainy growths or larger, cauliflower-like clusters. Plantar warts can be painful, especially while walking or standing, as they press into the skin and nerves. Despite their viral origin, they are not highly contagious and are more likely to develop in individuals with weakened immune systems or through direct contact with contaminated surfaces. If you have a plantar wart, it is suggested that you consult a podiatrist who can offer you the treatment option that is right for you.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Roy Rothman, DPM from Florida. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
Treatment
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see the fleshy wart. A podiatrist should only be consulted if there is an excessive amount of pain. Plantar warts are not cancerous or dangerous, but they can affect your walking and continually reappear. Anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin to make tiny blood clots visible and examine the inside of warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. Although plantar warts usually do not require an excessive amount of treatment, there are ways to go about removing them. A common method is to freeze them off using liquid nitrogen, removing them using an electrical tool, or burning them off via laser treatment. For a less invasive treatment option, topical creams can be used through a doctor’s prescription. This treatment method takes more time, however. Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places. Avoid this especially if you have open sores or cuts on your feet. It is also important to avoid direct contact with warts in general, as they are highly contagious.
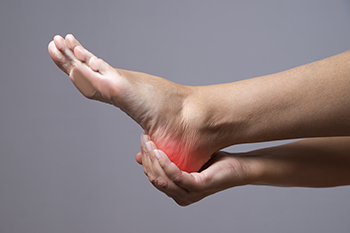
Heel pain can stem from various factors, including plantar fasciitis, Achilles tendonitis, heel bursitis, Haglund’s deformity, heel spurs, or even stress fractures. Symptoms often manifest as sharp or dull pain, particularly when walking or standing, localized around the heel or bottom of the foot. Risk factors include obesity, wearing improper footwear, and overuse during activities like running, and age. Prevention strategies involve wearing supportive shoes, maintaining a healthy weight, stretching the calf and foot muscles regularly, and avoiding sudden increases in physical activity. Treatment may include rest, stretching exercises, custom orthotic inserts, or in severe cases, surgery. A podiatrist can offer a tailored treatment plan by diagnosing the underlying cause of heel pain and providing targeted interventions. If you have heel pain, it is suggested that you schedule an appointment with a podiatrist for relief options.
Many people suffer from bouts of heel pain. For more information, contact Roy Rothman, DPM of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in DeBary, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
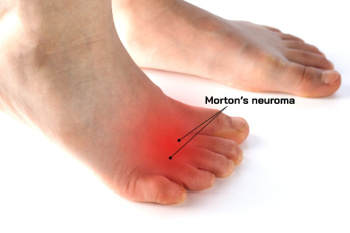
Morton's neuroma is a painful condition characterized by a thickening of the tissue surrounding the nerves leading to the toes, often resulting in a sensation akin to stepping on a pebble. It primarily affects the ball of the foot, typically between the third and fourth toes, and is more common in women and those who wear tight or high-heeled shoes. Prevention strategies include wearing properly fitting footwear with adequate support and cushioning. Diagnosis involves a physical examination, possibly supplemented by imaging tests, such as MRI scans or ultrasounds. Treatment options range from conservative measures such as custom-made orthotics and steroid injections to surgical removal of the affected tissue. If you have this type of foot discomfort, it is suggested that you schedule an appointment with a podiatrist for an accurate diagnosis and treatment plan.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Roy Rothman, DPM of Florida. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Morton’s neuroma, (also referred to as Morton’s metatarsalgia, Morton’s neuralgia, plantar neuroma or intermetatarsal neuroma) is a condition that is caused when the tissue around one of the nerves between your toes begins to thicken. This thickening can result in pain in the ball of the foot. Fortunately, the condition itself is not cancerous.
Morton’s neuroma affects women more often than men with a ratio of 4:1. It tends to target women between the age of 50 and 60, but it can occur in people of all ages. There are some risk factors that may put you at a slightly higher risk of developing the condition. People who often wear narrow or high-heeled shoes are often found to be linked to Morton’s neuroma. Additionally, activities such as running or jogging can put an enormous amount of pressure on the ligament and cause the nerve to thicken.
There usually aren’t any outward symptoms of this condition. A person who has Morton’s neuroma may feel as if they are standing on a pebble in their shoe. They may also feel a tingling or numbness in the toes as well as a burning pain in the ball of their foot that may radiate to their toes.
In order to properly diagnose you, the doctor will press on your foot to feel for a mass or tender spot. He may also do a series of tests such as x-rays, an ultrasound, or an MRI. X-rays are usually done to rule out any other causes for your foot pain such as a stress fracture. Ultrasounds are used to reveal soft tissue abnormalities that may exist, such as neuromas. Your podiatrist may want to use an MRI in order to visualize your soft tissues.
There are three main options for treatment of Morton’s neuroma: Injections, decompression surgery, and removal of the nerve. Injections of steroids into the painful area have been proven to help those with Morton’s neuroma. Decompression surgery has been shown to relieve pressure on the affected nerve by cutting nearby structures such as the ligaments in the foot. Another treatment option would be to surgically remove the growth to provide pain relief.
If you suspect that you have Morton’s neuroma you should make an appointment with your podiatrist right away. You shouldn’t ignore any foot pain that lasts longer than a few days, especially if the pain does not improve.
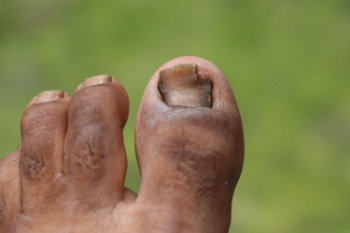
Toenail fungus, also known as onychomycosis, is more than just a cosmetic concern. It is a chronic problem that can cause discomfort and affect quality of life. It occurs when fungi infect the toenail, often thriving in warm, moist environments like sweaty shoes or locker rooms. Factors such as poor hygiene, a compromised immune system, aging, or underlying health conditions like diabetes can increase the risk of toenail fungus. The infection typically begins as a white or yellow spot under the nail, gradually spreading and thickening the nail, causing brittleness, discoloration, and even odor. Individuals who frequently wear closed-toe shoes or have a history of nail trauma are particularly susceptible. If you have toenail fungus, it is suggested that you consult a podiatrist for a proper diagnosis and management. Treatment can include prescribed topical or oral antifungal medications, laser therapy, or surgical intervention, tailored to the severity of the condition.
For more information about treatment, contact Roy Rothman, DPM of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
 Pregnancy, particularly during the third trimester, can contribute to pain in the front of the foot. This discomfort is mostly because of natural weight gain and the resulting increase in pressure on the feet. Additionally, hormonal changes during pregnancy cause the ligaments in the body to relax and stretch in preparation for childbirth, which can lead to a spreading of the feet and a decrease in arch support. This combination of factors can strain the forefoot and lead to conditions like plantar fasciitis, which results in pain and inflammation in the ball of the foot or heel. Podiatrists, or foot doctors, can provide personalized advice on how to manage this pain. Suggestions may include wearing supportive footwear, custom orthotics, and engaging in gentle foot exercises. If you are pregnant and experiencing foot pain, it is suggested that you consult a podiatrist.
Pregnancy, particularly during the third trimester, can contribute to pain in the front of the foot. This discomfort is mostly because of natural weight gain and the resulting increase in pressure on the feet. Additionally, hormonal changes during pregnancy cause the ligaments in the body to relax and stretch in preparation for childbirth, which can lead to a spreading of the feet and a decrease in arch support. This combination of factors can strain the forefoot and lead to conditions like plantar fasciitis, which results in pain and inflammation in the ball of the foot or heel. Podiatrists, or foot doctors, can provide personalized advice on how to manage this pain. Suggestions may include wearing supportive footwear, custom orthotics, and engaging in gentle foot exercises. If you are pregnant and experiencing foot pain, it is suggested that you consult a podiatrist.
Pregnant women with swollen feet can be treated with a variety of different methods that are readily available. For more information about other cures for swollen feet during pregnancy, consult with Roy Rothman, DPM from Florida. Our doctor will attend to all of your foot and ankle needs.
What Foot Problems Can Arise During Pregnancy?
One problem that can occur is overpronation, which occurs when the arch of the foot flattens and tends to roll inward. This can cause pain and discomfort in your heels while you’re walking or even just standing up, trying to support your baby.
Another problem is edema, or swelling in the extremities. This often affects the feet during pregnancy but tends to occur in the later stages.
How Can I Keep My Feet Healthy During Pregnancy?
If you have any questions please feel free to contact our office located in DeBary, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.